Autosomal recessive genetic disorder caused by a single nucleotide mutation of the haemoglobin ß-unit, from glutamic acid to valine. The resulting mutant haemoglobin S (HbS) is prone to distortion in cooler or hypoxic conditions, turning into a sickle shape. This damages the erythrocyte causing haemolysis.
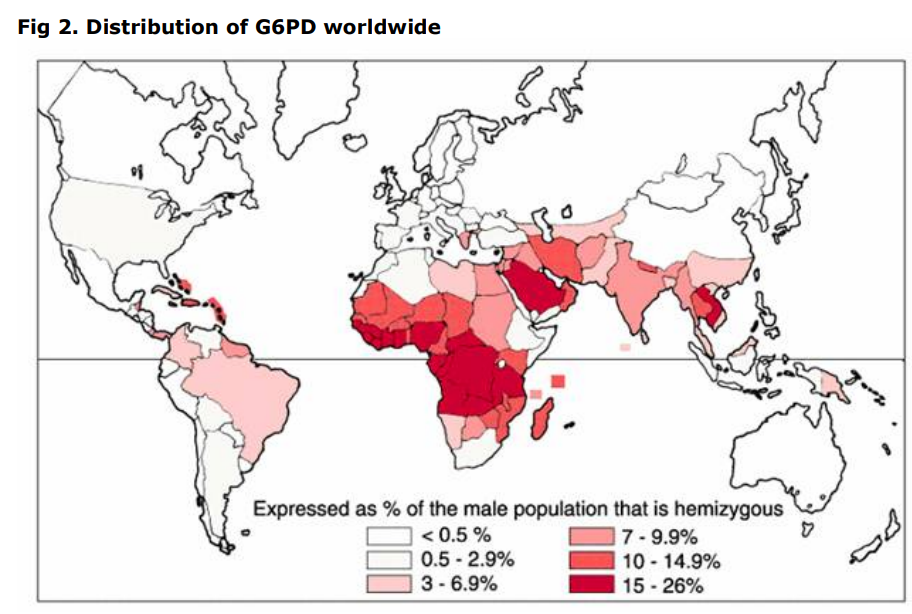
The gene is more common among Africans and is occasionally seen in races from the Middle East and South Asia. Its existence is due to protection from malaria seen in sickle cell trait (the heterozygote form), due to shortened red cell lifespan.
You can of course get combinations of sickle cell with other genetic haemoglobin disorders.
Triggers for sickling include cold environment, acidosis, hypoxia and hyperviscosity eg dehydration. Blood flow in capillaries is impaired by the damaged red cells, which leads to a vicious cycle of increased tissue acidosis and hypoxia. Infarction may occur.
Diagnosis
Can be diagnosed even in newborns. Sickle test followed by haemoglobin electrophoresis.
Screening programmes exist in some countries, so that prophylactic oral penicillin can get started early, preventing sepsis.
Clinical
Presents in infancy or early childhood, often with episodes of painful, swollen hands or feet (hand-foot syndrome). The neonate with its high proportion of Haemoglobin F does not get symptoms until there is enough abnormal haemoglobin A produced for red cells to start to sickle.
Acute Crisis
- Pain
- Chest syndrome
- Aplastic crisis
- Gut crisis
- Stroke
- Priapism
- Sepsis (may precipitate crisis or complicate it)
Pain
Pain can be widespread, but particularly involves bones, the spine, the chest.
Acute Chest syndrome
Can mimic pneumonia, with unilateral or bilateral signs of consolidation, pleuritic pain, and hypoxia. Pain is in chest wall, thoracic spine and upper abdomen. Leads to hypoventilation, causing vicious cycle of atelectasis and subsequently worse sickling. High mortality, so low threshold of suspicion.
- Hypoxia should be managed aggressively, with respiratory support if necessary.
- Antibiotics in infection contributing.
- Avoid diuretics – signs may suggest pulmonary oedema, but likely to exacerbate hyperviscosity.
Aplastic Crisis
Usually secondary to Erythrovirus B19 (formerly known as parvovirus B19) infection, which can trigger transient bone marrow arrest. So sudden drop in haemoglobin with an absence of reticulocytes. Classic “slapped cheek” appearance may never become apparent. Can affect multiple members of a family simultaneously. Differential is spleen sequestration.
Abdominal crisis
Manifest as anorexia, abdominal pain, distension. Usually not diarrhoea or vomiting. Usually not rebound. Bowel sounds usually quiet.
- Girdle or Mesenteric syndrome – ileus with vomiting. Associated with liver enlargement and bilateral basal consolidation.
- Differential includes appendicitis, biliary colic or cholecystitis, ischaemic colitis.
Stroke
Typically affects middle cerebral artery territory but may affect any region of the brain; may be transient or permanent. Seizures may occur. Predictive factors are:
- Previous TIA/stroke
- Chest syndrome
- Hypertension
- Family history of SCD related stroke
- Low HbF and/or low total haemoglobin
- Doppler velocities >200cm/sec in children
Differential is meningitis, subarachnoid haemorrhage (associated with multiple intracranial aneurysms).
Sequestration syndromes
- Splenic sequestration – Seen in infants and young children. Precipitated by fever or dehydration. Symptoms are:
- Abdominal pain/distension
- Rapidly expanding spleen (may or may not be painful)
- Shock, pallor due to drop in haemoglobin (but high reticulocytes cf aplastic crisis)
- Management is by fluid resuscitation with blood (type specific/O negative if necessary).
- Hepatic sequestration: similar to splenic, although less shock, and possibly jaundice along with enlarging liver.
- Priapism: =sustained painful erection. Potentially leads to peripheral gangrene, else cavernosal fibrosis and hence impotence. A urological emergency. Management:
- Warm bath, hydration, analgesia
- Catheterize if unable to urinate
- Sedation eg diazepam
- Aspiration + irrigation – ideally within 4-6hrs of onset. Else shunt.
- Top-up transfusion may be considered if unstable with other sickle related problems (aiming for Hb 10-12g/dl).
- Sepsis. Children are relatively immunocompromised due to functional hyposplenism from recurrent spleen infarction. This increases susceptibility to capsulated organisms eg pneumococcus, salmonella, haemophilus.
- Yersinia is a particular risk in children on desferrioxamine. Causes diarrhoea.
Management
- Analgesia, aiming to get rapid symptom control with IV bolus doses of opiates eg morphine, diamorphine ideally within 30 minutes of admission, followed by infusion or regular oral doses. Paracetamol and non-steroidal anti-inflammatories may be synnergistic.
- Oxygen, esp for acute chest syndrome. Debatable if effective for other problems.
- Hydration, even hyperhydration eg 150% normal daily requirements, IV if necessary. Impairment of renal concentrating power may contribute to dehydration.
- Warm environment
- Identification and treatment of infection. Give treatment doses of penicillin (else erythromycin) even if no specific agent identified.
- Treat with IV antibiotics if severe symptoms/signs
- Add macrolide eg clarithromycin if chest symptoms
- Treat empirically for Yersinia with ciprofloxacin if diarrhoea on desferrioxamine.
- Folic acid (should be on already)
Transfusion
Although anaemia is common in SCD, repeated transfusions lead to the possible complications of:
- Allo-immunization
- Iron overload
Hence top up transfusion is only used for acute symptomatic anaemia eg cardiac failure, severe sequestration or pre-operatively. Do not transfuse above Hb 11g/dl. Regular transfusions have a prophylactic role – see on-going treatment below.
Hyperhaemolysis is a life threatening complication of red cell transfusion in sickle cell disease. Can be acute (within 7 days of transfusion) or delayed. Affects not just transfused but autologous cells so Hb can drop below previous level. Fever, haemogobinuria as usual; negative DAT, reticulocytopenia seen (cf parvo). Cover subsequent transfusion with IVIG and steroids; use erythropoietin to maintain. For elective surgery, prophylactic postop CPAP has been used without transfusion. Risk factors poorly defined.
Exchange transfusion
Undertaken to rapidly reduce the percentage of sickle cells in the circulation where life-threatening eg severe chest syndrome, stroke, multi-organ failure. The aim is to reduce %HbS to <20%. Complications are common eg fluid overload, transfusion reaction.
Other Treatments
- Pneumococcal prophylaxis is essential for all children. Polysaccharide vaccine should be offered with repeat doses as per Green book.
- Folic acid
- Hepatitis B immunization
- Splenectomy for recurrent splenic sequestration.
On-going treatment
Consider for:
- Recurrent or stuttering priapism (etilefrine orally is another option here)
- Stroke/TIA
- Chronic organ damage eg renal failure
- Failure to thrive
- Intractable crises
Options:
- Regular transfusions. The aim is to keep %HbS <25%. Compared with exchange transfusion, regular transfusions are just as good at reducing complications, are less challenging in terms of vascular access, involve less donor exposure, but cause more iron accumulation.
- Hydroxyurea. Reduces frequency of crises and transfusion requirements, improves growth. Trials ongoing. Long term risks need to be clarified (toxicity, mutagenicity, teratogenicity).
- Bone marrow transplant
Iron overload and chelation therapy
Iron overload can be monitored by means of Ferritin levels. Chelation therapy should commence at ferritin levels of 1000mcg/l, with desferrioxamine (desferal) the chelator of choice. Treatment should include vitamin C. Ophthalmological, audiological and cardiological review is necessary.