Rare in developed world now, still common in underdeveloped world, or at least in underdeveloped communities eg Aboriginal Australians. Prob also genetic susceptibility.
Caused by Group A streptococcus. Important cause of acquired heart valve disease. Can recur.
Probably cross reactivity between specific Group A strep M proteins and human tissues.

Diagnosis
Jones criteria:
- Major
- Carditis eg new murmur. Mitral most commonly, classically apical blowing pan-systolic. Aortic next most common.
- Arthritis esp large joints. Migratory.
- Subcutaneous nodules – these are the most uncommon major criterium (in Turkish study of over 1000 cases there were none with nodules). Typically over extensor surfaces of joints, 0.5-2cm, symmetrical.
- Sydenhams chorea
- Erythema marginatum – not specific to rheumatic fever. Seen in 0.4% of Turkish study patients. Serpiginous or annual eruption, can look similar to erythema multiforme. Provoked by warmth eg bath. Non pruritic.
- Minor
- Fever
- Arthralgia
- Prolonged PR interval on ECG
- Elevated CRP/ESR
- 2 major or 1 major plus 2 minor, plus confirmation of group A streptococcal infection eg positive culture, high ASO titre sufficient for diagnosis. Modified Jones takes into account background incidence.
Note that initial infection may be subclinical eg pharyngitis, erysipelas. Symptoms of rheumatic fever develop 10 days to several weeks later. Chorea can appear months later. Low threshold for echo as carditis can also be subclinical.
Established criteria for rheumatic valvulitis – Gewitz 2015
Treatment
Antibiotics – Treat with penicillin, this does not however affect clinical course but hopefully prevents further spread of that particular bug. Traditionally single dose intramuscular Penicillin G Benzathine.
NSAIDs for joint pain. Usually dramatic response, if not then reconsider diagnosis!
Valproate for chorea, possibly steroids – see Sydenham’s.
Aspirin and/or Steroids for carditis, but not much evidence. Diuretics, ACE inhibitors for cardiac failure.
Long term treatment
Recurrence with progression of valve damage is the main concern, and well recognized. Subclinical carditis improves in about 50% but definite risk of progression (mild definite and borderline RHD showed 26% and 9.8% echocardiographic progression respectively).
Regular intramuscular penicillin (benzathine pencillin G) every 2-3 weeks has the lowest recurrence rates but oral penicillin V more acceptable. Erythromycin or cephalexin if allergic.
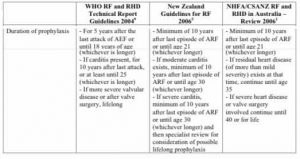
WHO recommendations:
- Rheumatic fever without carditis: 5 years after last attack or until age 18 (whichever is longer)
- Rheumatic fever with carditis but without residual disease: 10 years after last attack or until age 25 (whichever is longer)
- Residual valve disease or valve replacement: lifelong
American and Australian heart association guidelines vary slightly: